What to Expect in the Equine Emergency Room
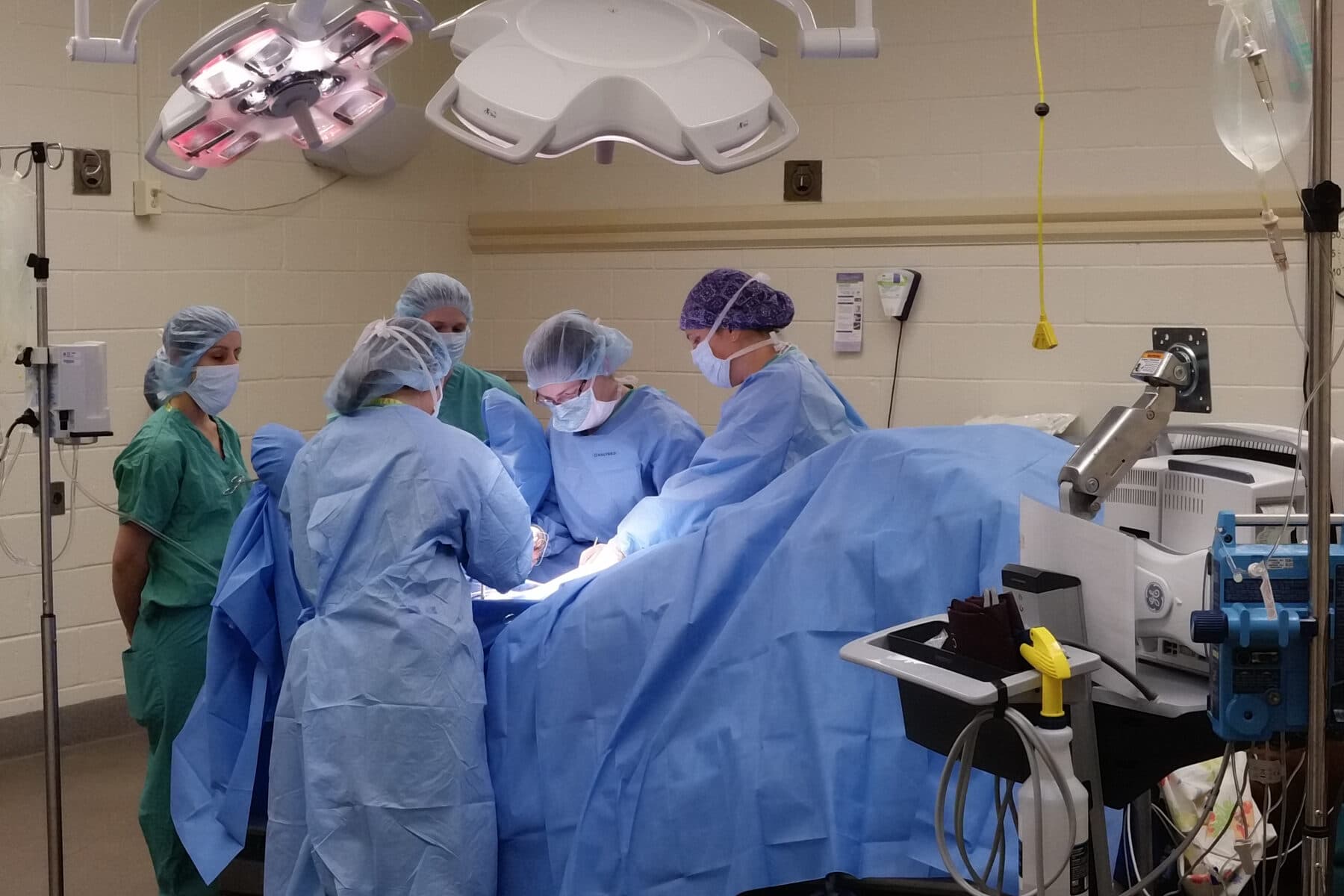
It is a truth universally acknowledged that if one owns a horse, that horse will eventually injure himself. Sometimes it’s just a mild scratch – easily treated in the barn. But sometimes the ailment is more serious, and then it’s time to call the vet. And what about the true emergencies, the ones that even the vet can’t treat on the farm? The ones that require surgery? That’s when it’s time for a trip to the equine hospital.
“Emergencies are the most stressful times,” stated Dr. Emily Schaefer, a Clinical Instructor of Equine Medicine at Virginia Tech's Marion duPont Scott Equine Medical Center (EMC) in Leesburg, Virginia. “If you show up for a more routine appointment, it’s less stressful. In an emergency situation, things are confusing and difficult to get a grip on.” They say knowledge is power, and knowing what to expect in an emergency situation can help keep things calm and under control.
The ER By the Numbers
The veterinarians at the Equine Medical Center are split into two teams - the Internal Medicine Faculty and the Surgery Faculty - and these two teams work together to help treat ill or injured horses based on their area of expertise. “Because we’re a team of specialists in medicine and surgery, we work differently and have different skills and tasks and a lot of the problems that we see alternate between teams,” Schaefer explained. “All departments here see a lot of cases together – it’s a really cohesive group.”
Schaefer shared that the EMC saw 561 emergency cases in 2018 – almost two emergencies per day on average. From there, she broke down those 561 cases by type of emergency.
What’s the most common type of emergency? Colic. “[Colic] accounts for almost half of all emergency cases at the EMC,” Schaefer said. “Those cases get worked up by both the internal medicine and surgical teams. We treat colic cases as best we can without surgery, but oftentimes there’s a decision-making point and that’s when we involve our surgeons and the whole teams works together to get those horses fixed.”
The second most common emergencies involve neonates, making up 10 percent of emergency cases at the EMC. “Neonates are a pretty big proportion of our emergency caseload and that is quite reflective of the emergent nature of sick babies. When a foal gets sick, they can get really sick really fast. Many veterinarians recognize that and if they see something starting to go south on the farm, they’re quick to refer which is absolutely the right decision.”

Next up on the list is lacerations, which accounted for seven percent of emergency cases last year. “If a horse can injure itself on something, it’s going to,” Schaefer joked. “These are the cases that surgeons generally see first – the surgeons come in and can usually get things patched up pretty quick.”
From there, the percentages continue to dwindle, with respiratory cases making up five percent, severe lameness and fevers of unknown origin making up 4 percent each, diarrhea/colitis three percent, cellulitis and eye injuries less than two percent each, and esophageal obstruction cases making up less than one percent.
When Emergency Strikes
The first instinct when faced with an equine medical emergency should be to call the horse’s primary veterinarian and have them assess the situation. “The patients we see are usually seen by their regular veterinarian first,” Schaefer confirmed. “Occasionally horses will come straight to us for evaluation, but oftentimes it’s the primary care veterinarian that takes a look at the horse and says, ‘This may be beyond what we can manage here in the barn. Let’s send this horse to a hospital.’”
“The field veterinarians are our first line of defense,” she continued. “There’s always a first line of communication between us and your veterinarian, and then ongoing communication during the process because they’re going to be the ones taking care of your horse when we send you home from the hospital.”
If the primary veterinarian reaches the point where he feels it’s time for the horse to go to the equine hospital “for further diagnostic and treatment,” it’s time to load up the trailer. “It could be that your veterinarian has made a diagnosis and knows exactly what’s going on, but the treatment isn’t appropriate on the farm. There are also plenty of times where it’s difficult to know what’s going on in the field when your toolbox is limited so they get referred for further diagnostics. That back-and-forth teamwork is really beneficial.”
At the Hospital
After arriving at the hospital and checking in at the admissions office, the equine hospital staff will usually take emergency cases to “drop one,” the hospital’s work-up stall. “This room is convenient in a lot of ways – it’s a big open space with padded walls and a door directly into the surgery suite,” Schaefer described. “Horses get worked up in here, we get a diagnosis if we can, and if they need to go to surgery right away we can anesthetize them, lift them up on the hoist, and go right into the surgery suite.”

“We call it ‘drop one’ because this is where we induce and recover from anesthesia – we literally “drop” the horse to the ground for general anesthesia – but they also wake up in this room,” she explained. “After surgery they come back in this room and sleep it off.”
Once the horse is settled in drop one, the veterinarian will start asking all sorts of questions to gather more information about the horse’s condition while a team member begins diagnostic work, including bloodwork and imaging. “The veterinarian wants to look at your horse right away, but they need a lot of information from you.” Schaefer stressed the importance of having salient information available so time won’t be wasted digging through paperwork or calling third parties for details. Information about symptoms, previous treatments, medications, travel history, and environment are all vital to helping the veterinarian treat in an emergency situation.
In the Surgical Suite
Not all cases brought to drop one will require surgery, but there are a few that are typically expedited straight to the surgical suite. The first and most common types of cases that go straight to surgery are colic that doesn’t respond to pain medication. “If you have a horse that’s colicking badly enough that he gets his pain meds and they either don’t work at all or it’s 20 to 30 minutes later and they’re getting painful again, that’s typically the threshold we use for taking horses to surgery.”
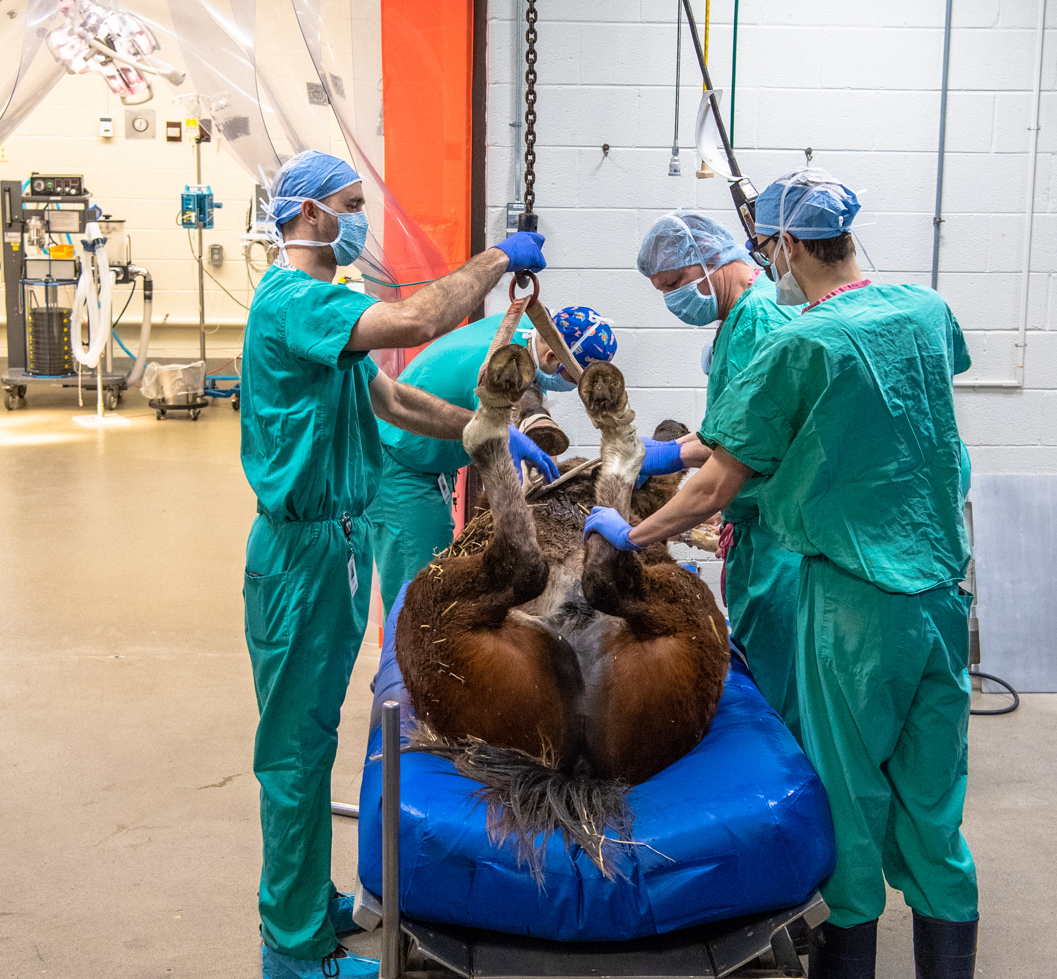
The second most common type of issues sent directly into surgery are wounds that involve a tendon or a joint. “A lot of lacerations and wounds can just be sewn up and put on antibiotics – taken care of relatively simply – unless they involve synovial structures that have those really thick, viscous fluid around them. If infection sets up in there that infection can get out of control quite fast, especially in horses, so we take them to surgery as an emergency situation.”
Dystocia is the third type of case that almost always require immediate emergency surgery. “Pregnant mares that start having their foal and can’t get it out can sometimes be resolved on the farm – it’s as simple as a flexed leg and your veterinarian can come out, fix that flexed knee, and pull the baby out,” said Schaefer. “Sometimes that’s not the case. Anywhere you’re coming from is a trailer ride away and the time frame to get a live foal out is really quite short, so they also have a very low threshold for being sent into surgery.”
Rest and Recovery
Because most horses in emergency situations aren’t eating or drinking, IV fluids and nutrients are crucial in the hours and days following a surgery or severe illness. “Whether or not they need surgery, horses that come to us on an emergency basis will probably require some period of critical care,” Schaefer explained.
“The crux of critical care is IV fluids. Horses need a lot of fluids - they’ll have four, five, even six 5-liter bags of fluids hanging from the ceiling because they are so big and go through fluids so fast. We can also give them the nutrition that they need through their IV. Because 47 percent of our cases are gastrointestinal, there’s usually a period of time after presentation that they’re not allowed to eat and we have to help them out somehow.” In addition to fluids, horses will be given dextrose and even amino acids via IV for fuel as well as vitamins like vitamin B and C and medications like anti-inflammatories, antibiotics, and gastroprotectants, all administered intravenously.
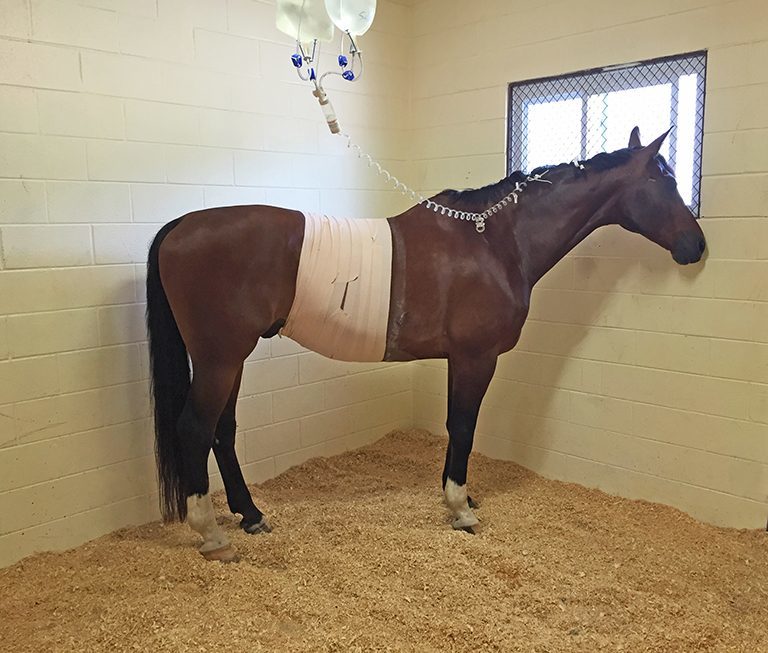
Critical care post-surgery also involves minute-by-minute monitoring of the horse by the hospital staff. “We’ve got to see how they’re responding to treatment and if they’re original presenting problem is still present then we either address it, treat it differently, or monitor it to its resolution.”
They say an ounce of prevention is a pound of cure, and Schaefer reiterated the importance of routine veterinary care and good horse management to help prevent emergencies. “The relationship you have with your veterinarian who comes out and sees your horse every year is going to be the most important part of preventing emergencies – deworming, vaccines – the things that seem mundane really are just that important.”
About Dr. Emily Schaefer
Dr. Emily Schaefer graduated cum laude from Saint Joseph’s University with a B.S. in Biology before earning her Veterinariae Medicinae Doctoris from the University of Pennsylvania in 2011. A Pennsylvania native, she returned to a large equine practice in southeastern Pennsylvania after completing an internship at Ohio State University. She worked for Unionville Equine Associates for three years before advancing her training with a residency in Large Animal Internal Medicine at the University of California, Davis. She joined the team at Marion duPont Scott Equine Medical Center in 2018. In addition to providing advanced diagnostics and treatment as part of the Internal Medicine team, she will focus on the assessment and support of critically ill horses and foals in an emergency setting.















