The 411 on Colic
This article originally appeared in the November/December 2018 issue of Eventing USA magazine.
As the season begins to turn, the temperature begins to drop, turnout time becomes more limited, schedules shift to accommodate the waning daylight and the possibility for a colicky horse increases. While the exact environmental causes of colic are not well understood, a commonly accepted theory is that any abrupt changes to a horse’s environment or schedule can increase the risk of colic.
Dr. Nathaniel White II, Professor Emeritus of Equine Surgery at the Virginia Tech Marion duPont Scott Equine Medical Center in Leesburg, Virginia, is a world-renowned expert in colic. “In the general equine population, between 4 and 10 percent are going to colic,” he stated. And while this percentage may seem relatively low, colic is still considered one of the most common equine medical diseases. Cause and Effect
While experts are still unsure which environmental triggers are to blame for colic, there are many possible intestinal changes associated with it. “One time we went through and tried to list all the different changes that occur and there were more than 80 different intestinal things that might cause colic,” explained White. “Then there are others like tying up or pneumonia that can cause the same behaviors.”
White described a study conducted by the Center where 1,000 horses were observed for occurrences of colic over a one-year period. “The most common colic was simple colic, and about 30 percent of those cases were owner-observed and got better quickly. They saw what looked like a sign of colic, like a gas pain, and then it disappeared.”
“About 80 percent of colic cases are simple, and we don’t know why even yet,” White elaborated. “We’re assuming gas, we’re assuming ulcers, we’re assuming some sort of motility thing that’s hurting. But usually they are easily treated.”
Impactions of the colon are the second most common type of colic, accounting for approximately seven percent of cases. White explained that impactions do not necessarily require surgery, and can and do pass on their own using treatments including mineral oil, electrolytes and a pain reliever like flunixin meglumine (Banamine).
The most severe cases of colic, including intestinal twists, displacements or those requiring surgery, made up four percent. “Some of the displacements we see that are more severe are where the large colon can get out of position, the small intestine can twist and get locked inside of itself, or the intestine can get into spaces where it’s not supposed to and get stuck.”
Recognizing the Signs
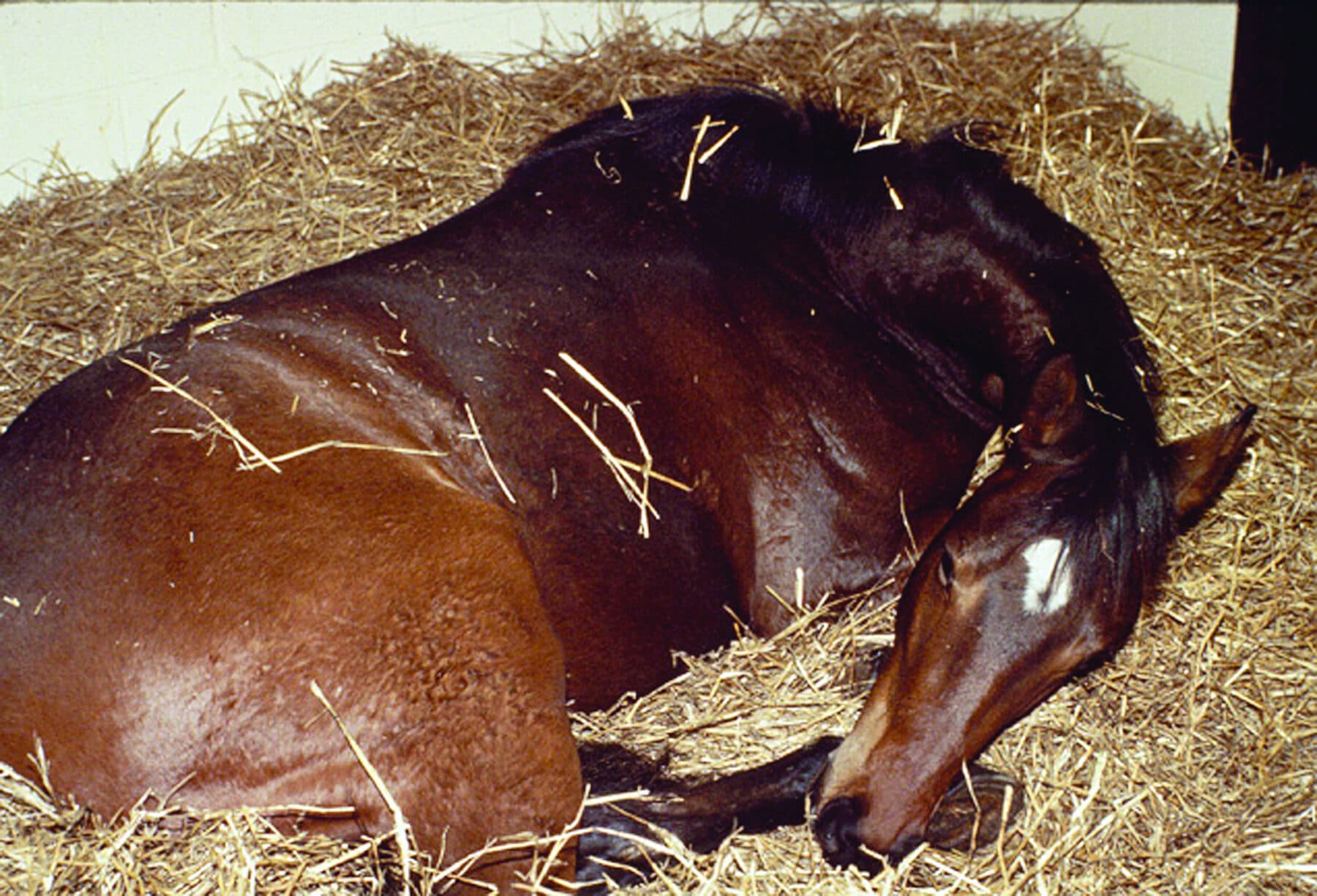
Early recognition and treatment are crucial with colic, where time can be of the essence. White explained that the earliest observable symptom is usually depression. “If their intestinal tract is upset, just like with us, they’re not going to be feeling very well.”
“The next thing they often show is evidence of pain,” he continued. “You can identify that by the position of their head and their expression. They paw, they walk around the stall looking uncomfortable, they may back into the corner. If the pain gets very severe, they’ll stretch out and then sometimes they go down and roll. Those are the main signs we see.
The speed at which colic can set in varies from case to case and can come on very quickly or be more drawn out. “We’ve seen horses in the show ring go down and immediately be severely colicking, but we also have some that just seem off for a while and are treated but still not quite right – they can go for days and either get worse or better.”
Call the Vet
If you notice your horse exhibiting symptoms of colic, the first thing you should do is call the vet. “Every colic is a potential emergency because it can be hard to tell if they need surgery,” White stated. “You shouldn’t wait to call the vet, even if it’s just to get advice. Even if you don’t have the vet come out, it’s better for them to know that you have a colicking horse so they can recommend what to do.”
In the Center’s study of 1,000 horses, 100 displayed symptoms of colic and only four of those cases required surgery. “The problem is, if you don’t recognize it early, it can be too late. Even a simple colic that starts out that way can very quickly turn into a surgical problem.”
In mild cases where both the owner and the vet feel comfortable with the vet recommending treatment over the phone, initial treatment with Banamine is one of the most common first steps. However, if the horse doesn’t improve after the administration of Banamine, something more serious may be going on.
“One treatment is called the ‘trailer ride cure,’” White joked, describing how people will put their horse on the trailer and bring him to the vet, only to have him step off the trailer saying, ‘Where’s my next meal?’ “We call that the trailer ride cure because the bouncing around or whatever the trailer ride does gets rid of the problem, but you can’t tell that’s going to happen.” And, if it doesn’t happen, you want your horse to be at the vet where he can get the care he needs.
“When a colicky horse comes to the hospital, there’s a system we go through to evaluate them, everything from temperature to mucus membranes, heart rate, rectal exam, and that’s standard and necessary,” said White. “When people come and they wonder what’s going on, we’re pretty much going through all the different evaluations to decide what we’re going to do.”
In the instances where surgery is necessary, time is of the essence. “That’s why every colic is an emergency,” White reiterated. “Even though it might be rare that a horse needs colic surgery, you can’t tell, the owner can’t tell, sometimes we have trouble telling what exactly is happening. There are situations where we’re not exactly sure what it is, but the horse is so painful that we go to surgery to make a diagnosis.”
What Happens in a Colic Surgery
Vets frequently don’t know what they’re going to encounter when they go in to perform a colic surgery. “We open them up along the midline and, depending on what we think the problem might be, we might open them up closer to the back end or closer to the front end, but there’s a standard place – in front of the umbilicus – and that’s where we make the incision,” White explained. “A lot of the abdomen isn’t visible, so you can bring out small intestine, you can bring out the large colon, you can bring out the cecum, but you can’t bring out all of it. You can’t bring out the stomach, you can see the liver, you can feel but not see the bladder.”
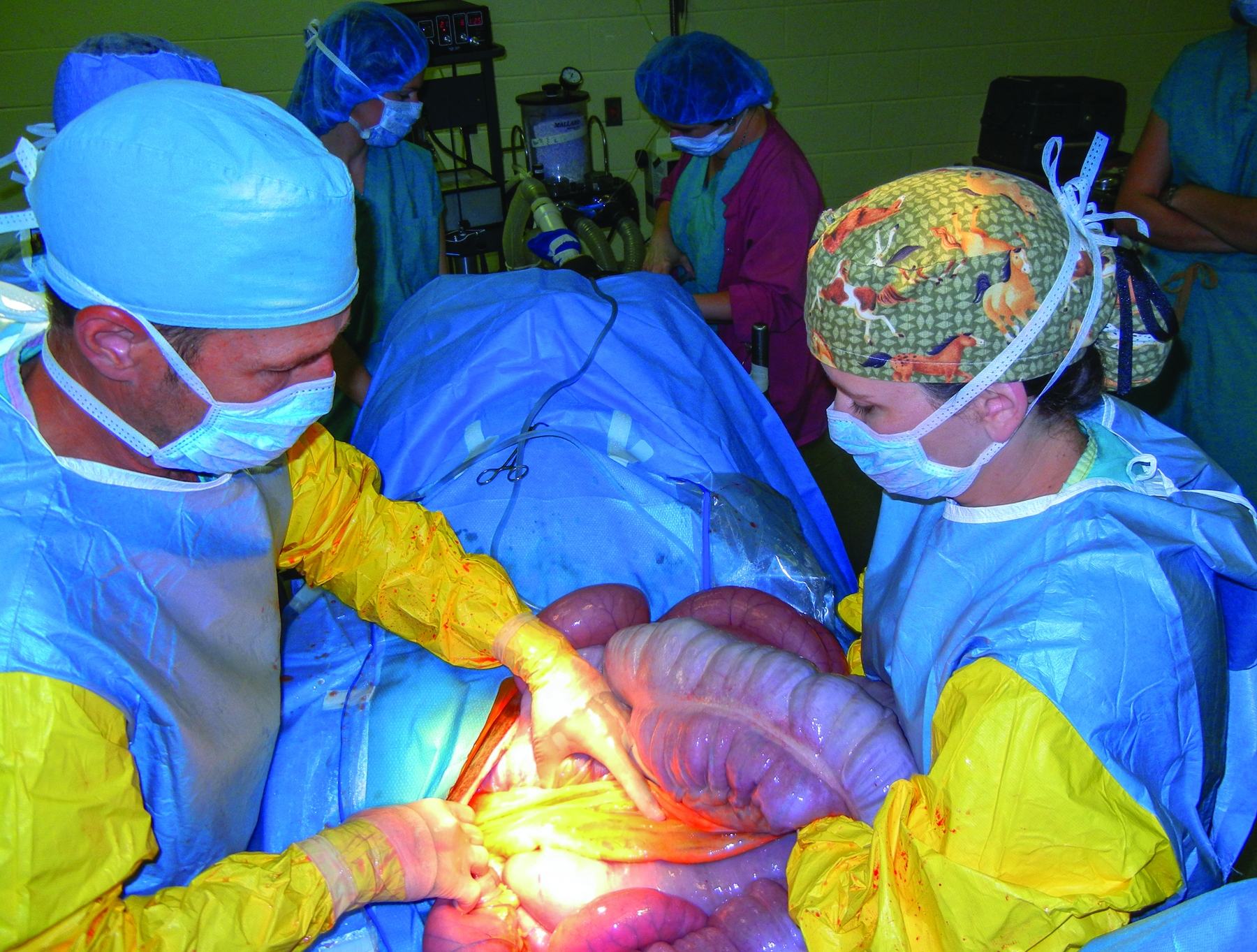
“The first thing the surgeon does is go in and check those structures, and sometimes the impaction or the twist is obvious and we work on that. I hope we make it look easy, but it’s not. It’s like a 55-gallon drum and you’re trying to figure out what’s going on by feel.”
White explained that the success rate on colic surgeries has gotten higher and higher as technology has improved and the veterinary knowledge has increased. “Over the years, given the training that we’ve gotten and that we give to our residents, surgery is expected to be a success unless the stage of the colic is too advanced.”
Recovery Mode
Depending on the type and severity of the colic and the resulting surgery, the recovery can be quick or it can be more drawn out. White described a case where the horse came in for colic surgery where the colon had become trapped by the spleen. They performed a successful surgery and the horse was back to race training in six weeks.
The good news is that horses who have colic surgery can and do return to their previous fitness level – their performance won’t be affected long-term. “Once they’ve recovered they can come back and perform at the same level.” For example, Mackenna Shea’s Landioso underwent colic surgery in August of 2015 and came back to compete at the Rolex Kentucky Three-Day Event in April of 2016.

Surgery is never without complications, and White shared that one of the most common post-colic surgery complications is adhesions of the intestine, where, depending on the health of the intestinal tissue, pieces of the intestine can get stuck to each other and cause an obstruction. “The real problem with the aftercare and recovery is if they get sick,” he continued, citing infection of the incision as another common post-operative complication. “When that happens, they sometimes require critical care in the hospital and then they have to rehabilitate.”
Stopping Colic Before it Starts
While the causes of colic are largely unknown, extensive study has revealed some common risk factors and corresponding prevention methods that can help reduce your horse’s risk for colic.
Diet is a significant factor in a horse’s risk for colic. Too much grain, which is not a natural part of the horse’s diet, can upset the digestive system. Additionally, the horse’s diet should consist of at least 70 percent forage.
Free access to water is another determining factor. Horses that suffer from water deprivation and dehydration are at a higher risk because the colon needs to absorb and retain fluid for digestion. Additionally, horses who have as much turnout as possible and are able to move freely are at a lower risk because movement assists with gut motility.
A strict daily feeding and exercise schedule has also been correlated with decreased colic risk. Additionally, increased monitoring during lifestyle changes, including those in diet, exercise, turnout or medical treatments is strongly recommended.
“If we could define the risk factors, this horse compared to that horse, and what it is that happened to that horse – exercise, trailering, water deprivation – that caused the colic, maybe we can prevent it. Those are the kind of important things that, if we could identify more of those, we can avoid the colic.”
About Nathaniel A. White, II, DVM, MS, Diplomate ACVS
Dr. White is a professor of surgery at the Marion duPont Scott Equine Medical Center. After receiving a doctor of veterinary medicine from Cornell University in 1971, he completed an internship and residency in surgery at the University of California at Davis from 1971 to 1973, and earned a master of science in pathology at Kansas State University in 1976. He is a Diplomate of the American College of Veterinary Surgeons (ACVS).
Dr. White, who has served on the faculties of both Kansas State University and the University of Georgia, joined the Marion duPont Scott Equine Medical Center in 1985, and held the position of Theodora Ayer Randolph Professor of Surgery at Virginia Tech from 1987 to 2003. He was the Jean Ellen Shehan Professor and Director from 2003-2012 and was named Professor Emeritus in Equine Surgery in September 2013.
A world-renowned expert in colic, Dr. White has authored several books on the topic including Equine Acute Abdomen and Handbook of Equine Colic as well as the surgical texts Current Techniques in Equine Surgery and Lameness and Current Practice of Equine Surgery. Dr. White’s research interests include pathophysiology of ischemia-reperfusion, epidemiology of colic, abdominal and orthopedic surgery, and treatment of orthopedic diseases.
Did you enjoy this article? Want to receive Eventing USA straight to your mailbox? Members receive Eventing USA as part of their USEA Membership or you can purchase individual issues from the USEA Shop.















